| Recently I had the opportunity to work with a woman 7 weeks postpartum. She had been experiencing heaviness and pressure in her vaginal area with walking, lifting, and prolonged standing. At her 6 week check in with her midwife, the midwife said she had a mild prolapse. Concerned about the discomfort and the inability to perform daily activities: lifting her 5 yr old and newborn, walking, standing...etc., and the potential further descent of her organs, she made an appointment with me. My evaluation confirmed her midwife's diagnosis of prolapse: a mild rectocele and urethrocele . In our session we worked on making her aware of habits that increase downward pressures which can contribute to prolapse, with the ultimate goal of reducing or eliminating such patterns. |
Habits that can affect the health of the pelvic floor
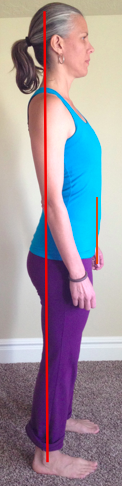
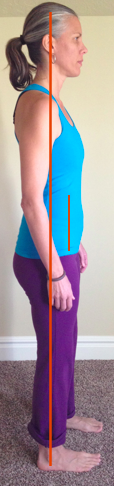
My client stood as most of us do, with her pelvis out in front of her. She also lifted her ribcage to bring her shoulders back. Ideally we should stand with our pelvis stacked over our ankles and our ribcage stacked over our pelvis; think about our functional core connection here: diaphragm, transversus abdominis, pelvic floor and deep back muscles. (For an educational read, get the book, The Pelvic Girdle by Diane Lee.) When the pelvis is out in front, we no longer have a neutral pelvis, which is important for the position of the pelvic organs (bladder, uterus) to have support of the pelvic ring below (notice in the pic above on the left, the bladder and uterus rest on the pubic bone). This means more grativational load on the fascia and ligaments leading to tissue failure (and descent of the organs). So my client learned how to stand.
Pulling in the gut to “look” slimmer freezes and shuts down the diaphragm, not to mention increases pressure in the cavities above and below. Read more about sucking in here: So my client learned how to breathe.
Tension in the pelvic floor
All muscles need to be able to contract and relax optimally. When the pelvis is out in front, the muscles in the pelvic floor are held in a shortened position. When there is increased pressure in the abdomen and pelvic cavities from sucking in, the pelvic floor muscles try to create balance by increasing contraction to maintain continence. Chronic tension means decreased blood flow, decreased oxygen, decreased waste removal = potential for pain signals. So, my client learned how to relax her pelvic floor.
Within a week she felt less heaviness and pressure in her vaginal area. She felt pressure only with heavy lifting. She possessed the education to continue her home program from the initial visit and we added gluteal strengthening to her program.
Two weeks later she returned to clinic reporting continued improvement. She was able to walk and perform yard work without any discomfort! She had a follow up visit with her midwife who reported upon exam significant reduction of prolapse! She was given additional functional movement reeducation for her home program. I will follow up with her in a month and more than likely discharge treatment.
Moral of the story is this: if you feel pressure or heaviness in your vaginal area postpartum (or at any time), get it taken care of, go see a pelvic health physical therapist. Or contact me for more information!












 RSS Feed
RSS Feed